Montelukast ile ili?kili Churg-Strauss sendromu
Meral UYAR1, Osman ELBEK1, Kemal BAKIR2, Yasemin K?BAR2, Nazan BAYRAM1, ?ner D?KENSOY1
1 Gaziantep ?niversitesi T?p Fak?ltesi, G???s Hastal?klar? Anabilim Dal?, Gaziantep,
2 Gaziantep ?niversitesi T?p Fak?ltesi, Patoloji Anabilim Dal?, Gaziantep.
?ZET
Montelukast ile ili?kili Churg-Strauss sendromu
Be? g?nd?r ?ks?r?k, nefes darl??? ve kan t?k?rme yak?nmas? ba?layan erkek hasta iki y?ld?r ast?m bron?iyale tan?s?yla flutikazon propionat ve salmeterol tedavisi kullanmaktayd?. ?ki hafta ?nce mevcut tedavisine inhaler steroid dozu azalt?lmadan montelukast eklendi?ini belirtti. Hastan?n serum eozinofil say?s? 1460/mm3 (%15) ve imm?nglobulin E d?zeyi 547 IU/mL idi. Toraks bilgisayarl? tomografisinde yamal? infiltrasyonlar saptanan hastan?n bronkoalveoler lavaj s?v?s?nda ve transbron?iyal biyopside eozinofilik inflamasyon tespit edildi. Churg-Strauss sendromu tan?s?yla prednizolon tedavisi ba?lanan hastada ?? ayl?k tedavi sonras?nda tam yan?t elde edildi. Hasta halen flutikazon propionat ve salmeterol tedavisi alt?nda sorunsuz izlenmektedir.
Anahtar Kelimeler: Churg-Strauss sendromu, ila?, l?kotrien resept?r antagonistleri, montelukast.
SUMMARY
Churg-Strauss syndrome related to montelukast
Meral UYAR1, Osman ELBEK1, Kemal BAKIR2, Yasemin K?BAR2, Nazan BAYRAM1, ?ner D?KENSOY1
1 Department of Chest Diseases, Faculty of Medicine, Gaziantep University, Gaziantep, Turkey.
2 Department of Pathology,Faculty of Medicine, Gaziantep University, Gaziantep, Turkey.
A young male with complaints of cough, dyspnea and hemoptysis was admitted. He was using fluticasone propionate and salmeterol for two years for his asthma. Leukotriene receptor antagonist was prescribed two weeks prior to his admission and no reduction of his inhaled steroid therapy was performed. Eosinophil count was detected as 1460/mm3 (15%) and immunoglobulin E level was 547 IU/mL. Thorax computerized tomography revealed patchy infiltration. Increased eosinophilic inflammation were detected in bronchoalveolar lavage fluid and transbronchial biopsy. He received prednisolone treatment for Churg-Strauss syndrome. Improvement was observed on three months follow up period. He has no complaint in his follow up.
Key Words: Churg-Strauss syndrome, drug, leukotriene receptor antagonist, montelukast.
Geli? Tarihi/Received: 26/02/2011 - Kabul Edili? Tarihi/Accepted: 21/04/2011
Churg-Strauss syndrome (CSS) is an important disease that requires aggressive treatment and careful monitoring. Although it is a rare disease the number of reports increased in the last two decades after leukotriene receptor antagonists (LRA) become available in the field of medicine (1,2,3,4,5,6,7,8). We present a young male with CSS in which the disease developed following a course of therapy with LRA without tapering his inhaled corticosteroid treatment, and he never used systemic corticosteroid.
CASE REPORT
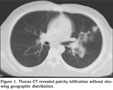
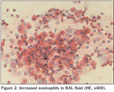
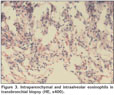
Eighteen year old male was admitted to hospital because of cough, dyspnea and hemoptysis. He was on inhaled corticosteroid and long acting bronchodilator treatment (fluticasone propionate and salmeterol 500/50 ?g twice daily) for two years for his asthma. For his progressing dyspnea the therapy was modified as adding montelukast for two weeks period without tapering his corticosteroid dosage six months prior to the admission. His first episode of hemoptysis was one month prior to the admission. Physical examination findings on presentation were as follows: body temperature, 36.7?C; pulse rate, 78 beats/minute; respiratory rate, 18 breath/minute; blood pressure, 120/70 mmHg; SpO2, 96%. Inspiratory and expiratory rhoncus were present on both lung fields. Laboratory findings were as follows: white blood cell, 9500/mm3; eosinophil count, 1460/mm3 (15%); hemoglobin, 15 g/dL; hematocrit, 45%; platelet count: 275.000/mm3; erythrocyte sedimentation rate, 8 mm/hour. His urinary analysis was normal. Immunoglobulin E level was 547 IU/mL (normal range: 0-100). Computerized tomography (CT) of paranasal sinus was compatible with bilateral maxillary sinusitis. Thorax CT revealed bilateral, patchy infiltration without showing geographic distribution with upper zone predominance (Figure 1). Skin prick test and ocular fundus examination were normal. His spirometric test results were compatible with moderate obstructive defect (FEV1: 47%, FVC: 66%, FEV1/FVC: 59%) and early reversibility response (29%) was present. Stool examination for parasite yielded no pathogen. Anti glomerular basement membrane, c and p-ANCA levels were also negative. Fiberoptic bronchoscopic examination was evaluated as normal tracheobronchial tree and bronchoalveolar lavage (BAL) and transbronchial biopsy was obtained from the lingula. Microbiologic studies of BAL were negative for a pathogenic agent. Cytopathological evaluation revealed increased eosinophils in BAL fluid and intraparenchymal and intraalveolar eosinophils in transbronchial biopsy (Figure 2, 3). The diagnosis of eosinophilic stage of CSS was made due to coexistance of asthma, with peripheral and BAL eosinophilia, infiltration on chest films, maxillary sinusitis, and the compatible biopsy findings. Patient was considered as eosinophilic phase of the disease because transbronchial biopsy was not compatible with vasculitis. Corticosteroid treatment with prednisolone 1 mg/kg was started. A significant radiological and clinical improvement was observed on three months follow up period.
DISCUSSION
In this report we presented a case diagnosed as CSS who used LRA but did not receive systemic corticosteroid treatment and also unchanged inhaled corticosteroid dose.
Three clinical stages for CSS have been described as prodromal, eosinophilic (vasculitic) and postvasculitic stage (9). The eosinophilic phase is diagnostic hallmark of early stage CSS (9). The BAL in the present case had striked eosinophilia (> 90%), and transbronchial biopsy was compatible with eosinophilic pneumonia only. There was no finding about kidney involvement.
There are many reports concerning the relationship between CSS and asthma medications such as zafirlukast, montelukast and pranlukast treatments (1,2,3,4,5,6,7,8). Food and Drug Administration (FDA) reported that 146 patients developed CSS in association with use of LRAs (6). These reports are mainly consisted of tapering of systemic corticosteroid treatment so concluded that main mechanism of CSS was considered to be an unmasking effect of the corticosteroid therapy. Another study who evaluated group of patients in respect to steroid usage or tapering concluded that most of the patient population were based on patients without alteration of steroid therapy and concluded that there is a casual relationship between LTA and CSS (10). There have been cases of CSS developing in asthmatic patients who had received the LRA zafirlukast and montelukast without recent tapering of corticosteroids (11,12). In the present case, there was no history of systemic corticosteroid usage, or dose reduction in the inhaled corticosteroid treatment when he was prescribed LRA. However, he was given LRA montelukast for two weeks, six months prior to his admission. Therefore, we believe that the hypothesis of tapering of corticosteroids unmasks the underlying CSS was not applicable to the present case. There is a case report about zafirlukast therapy and CSS in a patient who had no prior corticosteroid usage as our patient (13). Guilpain et al. also reported two cases of CSS due to montelukast who also did not receive systemic corticosteroid therapy before CSS diagnosis was made (14). So we believe that the drug-montelukast itself caused CSS contary to Jamaleddine et al. who declared that there is no evidence of LRAs as the development of CSS (1). Since, there have been many other drugs besides LRAs as responsible for the development of CSS (15). Another difference in the presented case is although clinical risk factors for CSS are reported to be moderately severe or severe asthma; our patient had mild asthma (13).
In conclusion we suggest that CSS is related to LTRA therapy rather than steroid tapering effect. CSS could be developed in patients receiving LTRA without tapering steroid therapy so attention about CSS development is necessary.
CONFLICT of INTEREST
None declared.
REFERENCES
- Jamaleddine G, Diab K, Tabbarah Z, et al. Leukotriene antagonists and the Churg-Strauss syndrome. Semin Arthritis Rheum 2002; 31: 218-27. [?zet]
- Michael AB, Murphy D. Montelukast-associated Churg-Strauss syndrome. Age Ageing 2003; 32: 551-2. [?zet] [PDF]
- Solans R, Bosch JA, Selva A, et al. Montelukast and Churg-Strauss syndrome. Thorax 2002; 57: 183-5. [?zet] [PDF]
- Boccagni C, Tesser F, Mittino D, et al. Churg-Strauss syndrome associated with the leukotriene antagonist montelukast. Neurol Sci 2004; 25: 21-2. [?zet]
- Kalyoncu AF, Karakaya G, Sahin AA, Artvinli M. Experience of 10 years with Churg-Strauss syndrome: an accompaniment to or a transition from aspirin-induced asthma? Allergol Immunopathol (Madr) 2001; 5: 185-90. [?zet]
- Weller PF, Plaut M, Taggart V, Trontell A. The relationship of asthma therapy and Churg-Strauss syndrome: NIH workshop summary report. J Allergy Clin Immunol 2001; 108: 175-83. [?zet]
- Ozlen B, Ozdemir L, Eskitutuncu B, Cevirme L, Kurtar N, Soy M, et al. Churg-Strauss syndrome associated with montelukast. Tuberk Toraks 2008; 56: 434-8. [?zet] [PDF]
- Kaliterna DM, Perkovic D, Radic M. Churg-Strauss syndrome associated with montelukast therapy. J Asthma 2009; 46: 604-5. [?zet]
- Mc Dannel DL, Muller BA. The linkage between Churg-Strauss syndrome and leukotriene receptor antagonists: Fact or fiction? Ther Clin Risk Manag 2005; 2: 125-40. [?zet] [Tam Metin] [PDF]
- Nathani N, Little MA, Kunst H, Wilson D, Thickett DR.Churg-Strauss syndrome and leukotriene antagonist use: a respiratory perspective. Thorax 2008; 63: 883-8. [?zet] [Tam Metin] [PDF]
- Katz RS, Papernik M. Zafirlukast and Churg-Strauss syndrome. JAMA 1998; 279: 1949-50.
- Tuggey JM, Hosker HS. Churg-Strauss syndrome associated with montelukast therapy. Thorax 2000; 55: 805-6. [?zet] [PDF]
- Soy M, Ozer H, Canataroglu A, Gumurdulu D, Erken E. Vasculitis induced by zafirlukast therapy. Clin Rheumatol 2002; 21: 328-9. [?zet]
- Guilpain
P, Viallard JF, Lagarde P, Cohen P, Kambouchner M, Pellegrin JL, et al.
Churg-Strauss syndrome in two patients receiving montelukast. Rheumatology
(Oxford)? 2002; 41: 535-9.
[?zet] [Tam Metin] [PDF] - Lilly CM, Churg A, Lazarovich M, Pauwels R, Hendeles L, Rosenwasser LJ, et al. Asthma therapies and Churg-Strauss syndrome. J Allergy Clin Immunol 2002; 109: 1-19. [?zet]
Yaz??ma Adresi (Address for Correspondence):
Dr. Meral UYAR,
Gaziantep ?niversitesi T?p Fak?ltesi,
G???s Hastal?klar? Anabilim Dal?,
27035 GAZ?ANTEP - TURKEY
e-mail: meraluyar1@yahoo.com